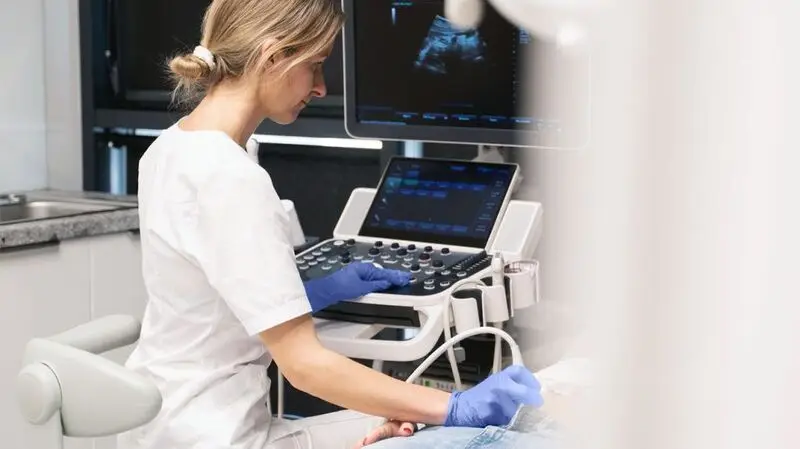
- Past research shows that a majority of endometriosis cases are misdiagnosed with other physical health or mental health issues.
- ACOG recently issued updated endometriosis clinical guidelines that, for the first time, offer comprehensive commendations for diagnosing endometriosis.
- The updated guidelines also address barriers to endometriosis care from racial and gender-identity bias, and emphasize the importance of shared decision making between the doctor and patient in endometriosis care.
According to the World Health Organization (WHO), about
Historically, endometriosis has been hard to diagnose because many of its symptoms, such as pain during the menstrual cycle or sex, chronic fatigue, nausea, and constipation vary and are shared with several other conditions, such as irritable bowel syndrome (IBS), ovarian cysts, and pelvic inflammatory disease (PID).
Past research shows that as much as
“Patients with endometriosis can experience significant delays in diagnosis,” Bliss Kaneshiro, MD, MPH, FACOG, professor in the Department of Obstetrics, Gynecology, and Women’s Health in the John A. Burns School of Medicine at the University of Hawaiʻi at Mānoa in Hawaii, told Medical News Today.
“For some, it takes years of experiencing pain before [an endometriosis] diagnosis is made. During this time, some patients can experience progression of disease which can affect their quality of life. Guidance that leads to quicker diagnosis can assist providers helping patients in a more timely manner.”
— Bliss Kaneshiro, MD, MPH, FACOG
Kaneshiro is one of the authors of updated endometriosis clinical guidelines issued by the American College of Obstetricians & Gynecologists (ACOG). For the first time, these guidelines offer comprehensive recommendations for diagnosing endometriosis.
The updated guidelines also address barriers to endometriosis care arising from racial and gender-identity bias, and emphasize the importance of shared decision making between the doctor and patient in endometriosis care.
ACOG’s updated endometriosis guidelines reportedly include comprehensive recommendations on diagnosis of the condition for the first time.
“Historically, endometriosis guidance has been fragmented, being discussed in pieces and suggestions rather than addressed in a unified, clear, structured way,” Jocelyn A. Carlo, MD, FACOG, director of gynecology and minimally invasive gynecologic surgeon at Hackensack Meridian Jersey Shore University Medical Center in New Jersey — who was not involved in the writing of these updated guidelines — told MNT.
“Having comprehensive criteria matters because endometriosis is not a one-dimensional disease. It presents differently from patient to patient, can affect multiple organ systems, and often overlaps with other pain symptoms.”
— Jocelyn A. Carlo, MD, FACOG
“A more complete framework helps clinicians think more broadly and systematically,” Carlo continued. “This kind of structure can improve consistency in evaluation, reduce variability in care, shorten time to diagnoses, and eventually lead to more timely treatment hopefully reducing the term sequelae of endometriosis and improving a woman’s quality of life.”
Adrian Balica, MD, a board-certified obstetrician-gynecologist at Atlantic Health — who was also not involved in the updating of these guidelines — commented that the new guidance validates endometriosis as a significant, disruptive disease that deserves earlier attention and more consistent care.
“The new clinical guidelines validate what many patients have been experiencing for years: endometriosis can cause both pelvic and extra-pelvic symptoms, and those symptoms are real, meaningful, and medically important,” Balica explained.
“The guidelines also support starting treatment based on a clinical diagnosis, which means patients do not have to wait for surgery or advanced imaging before receiving care. This allows clinicians to begin managing symptoms earlier even when treatments may be costly so patients can get relief sooner and avoid years of unnecessary suffering.”
— Adrian Balica, MD
The updated endometriosis guidelines also offer strategies to clinicians to help reduce barriers to endometriosis care caused by racial and gender-identification bias.
“Erroneous beliefs about biological differences between people of different races have contributed to racial [disparities] in endometriosis diagnosis,” Kaneshiro said. “Transgender men and other [genders] may face unique barriers when presenting for endometriosis care. We providers need to be aware of this.”
“Endometriosis has been under-recognized in marginalized and minoritized populations,” Steven Vasilev, MD, gynecologic oncologist specializing in endometriosis and founder of the Lotus Endometriosis Institute in Santa Monica, CA — who was not involved in the updating of these guidelines — told MNT. “Addressing disparities in awareness and evaluation is essential.”
“[I]t is clear that early and accurate evaluation should be available to all patients,” Vasilev continued. He said all patients should have “timely access to appropriate levels of expertise when symptoms suggest complex disease. Earlier recognition should lead to earlier accurate treatment — not simply earlier prescriptions.”
Additionally, ACOG’s updated guidelines place an emphasis on the importance of shared decision making between doctor and patients in endometriosis care.
“Patient centered care prioritizes the needs of each individual patient and acknowledges that different patients may experience endometriosis differently,” Kaneshiro said. “Our jobs as providers is to give patients the information they need to make a health care decision that is best for them.”
And within the updated guidelines, Carlo said she was most encouraged about the attention these guidelines bring to addressing women’s pelvic pain and menstrual symptoms.
“When a major organization like ACOG issues updated clinical guidance, it signals that endometriosis deserves a serious, structured, and evidence-based approach,” she explained.
“Increased awareness on the national level helps shift both patient and physician perspectives towards this complex and challenging disease. Most importantly this new guideline reflects that ACOG is hearing the voices of patients who have been advocating for better recognition and more responsive care,” Carlo added.
“These guidelines represent an important effort to improve awareness and reduce diagnostic delay. That intent deserves recognition. Moving away from normalization and dismissal of pelvic pain is progress. While reducing diagnostic delay is critically important, the question is how to balance earlier treatment with diagnostic precision in a structurally complex disease.”
— Steven Vasilev, MD
“The guidelines push the entire health care system and society to take a hard look at how often endometriosis is overlooked or minimized,” Balica added. “They call for greater awareness, better education, and more coordinated action to shorten the long delays patients face. And they underscore how debilitating symptoms can start very early in life, which makes early recognition and validation essential.”





