Drug Detail:Dacogen (Decitabine [ de-sit-a-been ])
Drug Class: Antimetabolites
Highlights of Prescribing Information
DACOGEN® (decitabine) for injection, for intravenous use
Initial U.S. Approval: 2006
Indications and Usage for Dacogen
DACOGEN is a nucleoside metabolic inhibitor indicated for treatment of adult patients with myelodysplastic syndromes (MDS) including previously treated and untreated, de novo and secondary MDS of all French-American-British subtypes (refractory anemia, refractory anemia with ringed sideroblasts, refractory anemia with excess blasts, refractory anemia with excess blasts in transformation, and chronic myelomonocytic leukemia) and intermediate-1, intermediate-2, and high-risk International Prognostic Scoring System groups. (1)
Dacogen Dosage and Administration
- Three Day Regimen: Administer DACOGEN at a dose of 15 mg/m2 by continuous intravenous infusion over 3 hours repeated every 8 hours for 3 days. Repeat cycle every 6 weeks. (2.1)
- Five Day Regimen: Administer DACOGEN at a dose of 20 mg/m2 by continuous intravenous infusion over 1 hour repeated daily for 5 days. Repeat cycle every 4 weeks. (2.1)
Dosage Forms and Strengths
For Injection: 50 mg of decitabine as a lyophilized powder in a single-dose vial for reconstitution. (3)
Contraindications
None. (4)
Warnings and Precautions
- Neutropenia and Thrombocytopenia: Perform complete blood counts and platelet counts. (5.1)
- Embryo-Fetal Toxicity: Can cause fetal harm. Advise patients of reproductive potential of the potential risk to a fetus and to use effective contraception (5.2, 8.1, 8.3)
Adverse Reactions/Side Effects
Most common adverse reactions (>50%) are neutropenia, thrombocytopenia, anemia, and pyrexia. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact Otsuka America Pharmaceutical, Inc. at 1-800-438-9927 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Use In Specific Populations
Lactation: Advise not to breastfeed. (8.2)
See 17 for PATIENT COUNSELING INFORMATION.
Revised: 11/2021
Full Prescribing Information
1. Indications and Usage for Dacogen
DACOGEN is indicated for treatment of adult patients with myelodysplastic syndromes (MDS) including previously treated and untreated, de novo and secondary MDS of all French-American-British subtypes (refractory anemia, refractory anemia with ringed sideroblasts, refractory anemia with excess blasts, refractory anemia with excess blasts in transformation, and chronic myelomonocytic leukemia) and intermediate-1, intermediate-2, and high-risk International Prognostic Scoring System groups.
2. Dacogen Dosage and Administration
2.3 Preparation and Administration
DACOGEN is a cytotoxic drug. Follow special handling and disposal procedures.1
Aseptically reconstitute DACOGEN with room temperature (20°C to 25°C) 10 mL of Sterile Water for Injection, USP. Upon reconstitution, the final concentration of the reconstituted DACOGEN solution is 5 mg/mL. You must dilute the reconstituted solution with 0.9% Sodium Chloride Injection or 5% Dextrose Injection prior to administration. Temperature of the diluent (0.9% Sodium Chloride Injection or 5% Dextrose Injection) depends on time of administration after preparation.
3. Dosage Forms and Strengths
For Injection: 50 mg of decitabine as a sterile, white to almost white lyophilized powder in a single-dose vial for reconstitution
5. Warnings and Precautions
5.1 Myelosuppression
Fatal and serious myelosuppression occurs in DACOGEN-treated patients. Myelosuppression (anemia, neutropenia, and thrombocytopenia) is the most frequent cause of DACOGEN dose reduction, delay, and discontinuation. Neutropenia of any grade occurred in 90% of DACOGEN-treated patients with grade 3 or 4 occurring in 87% of patients. Grade 3 or 4 febrile neutropenia occurred in 23% of patients. Thrombocytopenia of any grade occurred in 89% of patients with grade 3 or 4 occurring in 85% of patients. Anemia of any grade occurred in 82% of patients. Perform complete blood count with platelets at baseline, prior to each cycle, and as needed to monitor response and toxicity. Manage toxicity using dose-delay, dose-reduction, growth factors, and anti-infective therapies as needed [see Dosage and Administration (2.2)]. Myelosuppression and worsening neutropenia may occur more frequently in the first or second treatment cycles and may not necessarily indicate progression of underlying MDS.
5.2 Embryo-Fetal Toxicity
Based on findings from human data, animal studies and its mechanism of action, DACOGEN can cause fetal harm when administered to a pregnant woman [see Clinical Pharmacology (12.1) and Nonclinical Toxicology (13.1)]. In preclinical studies in mice and rats, decitabine caused adverse developmental outcomes including embryo-fetal lethality and malformations. Advise pregnant women of the potential risk to a fetus. Advise females of reproductive potential to use effective contraception while receiving DACOGEN and for 6 months following the last dose. Advise males with female partners of reproductive potential to use effective contraception while receiving treatment with DACOGEN and for 3 months following the last dose [see Use in Specific Populations (8.1, 8.3)].
6. Adverse Reactions/Side Effects
The following clinically significant adverse reactions are described elsewhere in the labeling:
- Myelosuppression [see Warnings and Precautions (5.1)]
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The safety of DACOGEN was studied in 3 single-arm studies (N =66, N =98, N =99) and 1 controlled supportive care study (N =83 DACOGEN, N =81 supportive care). The data described below reflect exposure to DACOGEN in 83 patients in the MDS trial. In the trial, patients received 15 mg/m2 intravenously every 8 hours for 3 days every 6 weeks. The median number of DACOGEN cycles was 3 (range 0 to 9).
Most Common Adverse Reactions: neutropenia, thrombocytopenia, anemia, fatigue, pyrexia, nausea, cough, petechiae, constipation, diarrhea, and hyperglycemia.
Adverse Reactions Most Frequently (≥1%) Resulting in Clinical Intervention and or Dose Modification in the Controlled Supportive Care Study in the DACOGEN Arm:
- Discontinuation: thrombocytopenia, neutropenia, pneumonia, Mycobacterium avium complex infection, cardio-respiratory arrest, increased blood bilirubin, intracranial hemorrhage, abnormal liver function tests.
- Dose Delayed: neutropenia, pulmonary edema, atrial fibrillation, central line infection, febrile neutropenia.
- Dose Reduced: neutropenia, thrombocytopenia, anemia, lethargy, edema, tachycardia, depression, pharyngitis.
Table 1 presents all adverse reactions occurring in at least 5% of patients in the DACOGEN group and at a rate greater than supportive care.
| DACOGEN N =83 (%) | Supportive Care N =81 (%) |
|
|---|---|---|
| Blood and lymphatic system disorders | ||
| Neutropenia | 75 (90) | 58 (72) |
| Thrombocytopenia | 74 (89) | 64 (79) |
| Anemia NOS | 68 (82) | 60 (74) |
| Febrile neutropenia | 24 (29) | 5 (6) |
| Leukopenia NOS | 23 (28) | 11 (14) |
| Lymphadenopathy | 10 (12) | 6 (7) |
| Thrombocythemia | 4 (5) | 1 (1) |
| Cardiac disorders | ||
| Pulmonary edema NOS | 5 (6) | 0 (0) |
| Eye disorders | ||
| Vision blurred | 5 (6) | 0 (0) |
| Gastrointestinal disorders | ||
| Nausea | 35 (42) | 13 (16) |
| Constipation | 29 (35) | 11 (14) |
| Diarrhea NOS | 28 (34) | 13 (16) |
| Vomiting NOS | 21 (25) | 7 (9) |
| Abdominal pain NOS | 12 (14) | 5 (6) |
| Oral mucosal petechiae | 11 (13) | 4 (5) |
| Stomatitis | 10 (12) | 5 (6) |
| Dyspepsia | 10 (12) | 1 (1) |
| Ascites | 8 (10) | 2 (2) |
| Gingival bleeding | 7 (8) | 5 (6) |
| Hemorrhoids | 7 (8) | 3 (4) |
| Loose stools | 6 (7) | 3 (4) |
| Tongue ulceration | 6 (7) | 2 (2) |
| Dysphagia | 5 (6) | 2 (2) |
| Oral soft tissue disorder NOS | 5 (6) | 1 (1) |
| Lip ulceration | 4 (5) | 3 (4) |
| Abdominal distension | 4 (5) | 1 (1) |
| Abdominal pain upper | 4 (5) | 1 (1) |
| Gastro-esophageal reflux disease | 4 (5) | 0 (0) |
| Glossodynia | 4 (5) | 0 (0) |
| General disorders and administrative site disorders | ||
| Pyrexia | 44 (53) | 23 (28) |
| Edema peripheral | 21 (25) | 13 (16) |
| Rigors | 18 (22) | 14 (17) |
| Edema NOS | 15 (18) | 5 (6) |
| Pain NOS | 11 (13) | 5 (6) |
| Lethargy | 10 (12) | 3 (4) |
| Tenderness NOS | 9 (11) | 0 (0) |
| Fall | 7 (8) | 3 (4) |
| Chest discomfort | 6 (7) | 3 (4) |
| Intermittent pyrexia | 5 (6) | 3 (4) |
| Malaise | 4 (5) | 1 (1) |
| Crepitations NOS | 4 (5) | 1 (1) |
| Catheter site erythema | 4 (5) | 1 (1) |
| Catheter site pain | 4 (5) | 0 (0) |
| Injection site swelling | 4 (5) | 0 (0) |
| Hepatobiliary disorders | ||
| Hyperbilirubinemia | 12 (14) | 4 (5) |
| Infections and infestations | ||
| Pneumonia NOS | 18 (22) | 11 (14) |
| Cellulitis | 10 (12) | 6 (7) |
| Candidal infection NOS | 8 (10) | 1 (1) |
| Catheter related infection | 7 (8) | 0 (0) |
| Urinary tract infection NOS | 6 (7) | 1 (1) |
| Staphylococcal infection | 6 (7) | 0 (0) |
| Oral candidiasis | 5 (6) | 2 (2) |
| Sinusitis NOS | 4 (5) | 2 (2) |
| Bacteremia | 4 (5) | 0 (0) |
| Injury, poisoning and procedural complications | ||
| Transfusion reaction | 6 (7) | 3 (4) |
| Abrasion NOS | 4 (5) | 1 (1) |
| Investigations | ||
| Cardiac murmur NOS | 13 (16) | 9 (11) |
| Blood alkaline phosphatase NOS increased | 9 (11) | 7 (9) |
| Aspartate aminotransferase increased | 8 (10) | 7 (9) |
| Blood urea increased | 8 (10) | 1 (1) |
| Blood lactate dehydrogenase increased | 7 (8) | 5 (6) |
| Blood albumin decreased | 6 (7) | 0 (0) |
| Blood bicarbonate increased | 5 (6) | 1 (1) |
| Blood chloride decreased | 5 (6) | 1 (1) |
| Protein total decreased | 4 (5) | 3 (4) |
| Blood bicarbonate decreased | 4 (5) | 1 (1) |
| Blood bilirubin decreased | 4 (5) | 1 (1) |
| Metabolism and nutrition disorders | ||
| Hyperglycemia NOS | 27 (33) | 16 (20) |
| Hypoalbuminemia | 20 (24) | 14 (17) |
| Hypomagnesemia | 20 (24) | 6 (7) |
| Hypokalemia | 18 (22) | 10 (12) |
| Hyponatremia | 16 (19) | 13 (16) |
| Appetite decreased NOS | 13 (16) | 12 (15) |
| Anorexia | 13 (16) | 8 (10) |
| Hyperkalemia | 11 (13) | 3 (4) |
| Dehydration | 5 (6) | 4 (5) |
| Musculoskeletal and connective tissue disorders | ||
| Arthralgia | 17 (20) | 8 (10) |
| Pain in limb | 16 (19) | 8 (10) |
| Back pain | 14 (17) | 5 (6) |
| Chest wall pain | 6 (7) | 1 (1) |
| Musculoskeletal discomfort | 5 (6) | 0 (0) |
| Myalgia | 4 (5) | 1 (1) |
| Nervous system disorders | ||
| Headache | 23 (28) | 11 (14) |
| Dizziness | 15 (18) | 10 (12) |
| Hypoesthesia | 9 (11) | 1 (1) |
| Psychiatric disorders | ||
| Insomnia | 23 (28) | 11 (14) |
| Confusional state | 10 (12) | 3 (4) |
| Anxiety | 9 (11) | 8 (10) |
| Renal and urinary disorders | ||
| Dysuria | 5 (6) | 3 (4) |
| Urinary frequency | 4 (5) | 1 (1) |
| Respiratory, thoracic and Mediastinal disorders | ||
| Cough | 33 (40) | 25 (31) |
| Pharyngitis | 13 (16) | 6 (7) |
| Crackles lung | 12 (14) | 1 (1) |
| Breath sounds decreased | 8 (10) | 7 (9) |
| Hypoxia | 8 (10) | 4 (5) |
| Rales | 7 (8) | 2 (2) |
| Postnasal drip | 4 (5) | 2 (2) |
| Skin and subcutaneous tissue disorders | ||
| Ecchymosis | 18 (22) | 12 (15) |
| Rash NOS | 16 (19) | 7 (9) |
| Erythema | 12 (14) | 5 (6) |
| Skin lesion NOS | 9 (11) | 3 (4) |
| Pruritis | 9 (11) | 2 (2) |
| Alopecia | 7 (8) | 1 (1) |
| Urticaria NOS | 5 (6) | 1 (1) |
| Swelling face | 5 (6) | 0 (0) |
| Vascular disorders | ||
| Petechiae | 32 (39) | 13 (16) |
| Pallor | 19 (23) | 10 (12) |
| Hypotension NOS | 5 (6) | 4 (5) |
| Hematoma NOS | 4 (5) | 3 (4) |
In a single-arm MDS study (N=99), DACOGEN was dosed at 20 mg/m2 intravenously, infused over one hour daily, for 5 consecutive days of a 4-week cycle. Table 2 presents all adverse reactions occurring in at least 5% of patients.
| DACOGEN N =99 (%) |
|
|---|---|
|
|
| Blood and lymphatic system disorders | |
| Anemia | 31 (31) |
| Febrile neutropenia | 20 (20) |
| Leukopenia | 6 (6) |
| Neutropenia | 38 (38) |
| Pancytopenia | 5 (5) |
| Thrombocythemia | 5 (5) |
| Thrombocytopenia | 27 (27) |
| Cardiac disorders | |
| Cardiac failure congestive | 5 (5) |
| Tachycardia | 8 (8) |
| Ear and labyrinth disorders | |
| Ear pain | 6 (6) |
| Gastrointestinal disorders | |
| Abdominal pain | 14 (14) |
| Abdominal pain upper | 6 (6) |
| Constipation | 30 (30) |
| Diarrhea | 28 (28) |
| Dyspepsia | 10 (10) |
| Dysphagia | 5 (5) |
| Gastro-esophageal reflux disease | 5 (5) |
| Nausea | 40 (40) |
| Oral pain | 5 (5) |
| Stomatitis | 11 (11) |
| Toothache | 6 (6) |
| Vomiting | 16 (16) |
| General disorders and administration site conditions | |
| Asthenia | 15 (15) |
| Chest pain | 6 (6) |
| Chills | 16 (16) |
| Fatigue | 46 (46) |
| Mucosal inflammation | 9 (9) |
| Edema | 5 (5) |
| Edema peripheral | 27 (27) |
| Pain | 5 (5) |
| Pyrexia | 36 (36) |
| Infections and infestations | |
| Cellulitis | 9 (9) |
| Oral candidiasis | 6 (6) |
| Pneumonia | 20 (20) |
| Sinusitis | 6 (6) |
| Staphylococcal bacteremia | 8 (8) |
| Tooth abscess | 5 (5) |
| Upper respiratory tract infection | 10 (10) |
| Urinary tract infection | 7 (7) |
| Injury, poisoning and procedural complications | |
| Contusion | 9 (9) |
| Investigations | |
| Blood bilirubin increased | 6 (6) |
| Breath sounds abnormal | 5 (5) |
| Weight decreased | 9 (9) |
| Metabolism and nutrition disorders | |
| Anorexia | 23 (23) |
| Decreased appetite | 8 (8) |
| Dehydration | 8 (8) |
| Hyperglycemia | 6 (6) |
| Hypokalemia | 12 (12) |
| Hypomagnesemia | 5 (5) |
| Musculoskeletal and connective tissue disorders | |
| Arthralgia | 17 (17) |
| Back pain | 18 (18) |
| Bone pain | 6 (6) |
| Muscle spasms | 7 (7) |
| Muscular weakness | 5 (5) |
| Musculoskeletal pain | 5 (5) |
| Myalgia | 9 (9) |
| Pain in extremity | 18 (18) |
| Nervous system disorders | |
| Dizziness | 21 (21) |
| Headache | 23 (23) |
| Psychiatric disorders | |
| Anxiety | 9 (9) |
| Confusional state | 8 (8) |
| Depression | 9 (9) |
| Insomnia | 14 (14) |
| Respiratory, thoracic and mediastinal disorders | |
| Cough | 27 (27) |
| Dyspnea | 29 (29) |
| Epistaxis | 13 (13) |
| Pharyngolaryngeal pain | 8 (8) |
| Pleural effusion | 5 (5) |
| Sinus congestion | 5 (5) |
| Skin and subcutaneous tissue disorders | |
| Dry skin | 8 (8) |
| Ecchymosis | 9 (9) |
| Erythema | 5 (5) |
| Night sweats | 5 (5) |
| Petechiae | 12 (12) |
| Pruritus | 9 (9) |
| Rash | 11 (11) |
| Skin lesion | 5 (5) |
| Vascular disorders | |
| Hypertension | 6 (6) |
| Hypotension | 11 (11) |
No overall difference in safety was detected between patients >65 years of age and younger patients in these MDS trials. No significant differences in safety were detected between males and females. Patients with renal or hepatic dysfunction were not studied. Insufficient numbers of non-White patients were available to draw conclusions in these clinical trials.
Serious adverse reactions that occurred in patients receiving DACOGEN not previously reported in Tables 1 and 2 include:
- Allergic Reaction: hypersensitivity (anaphylactic reaction)
- Blood and Lymphatic System Disorders: myelosuppression, splenomegaly
- Cardiac Disorders: myocardial infarction, cardio-respiratory arrest, cardiomyopathy, atrial fibrillation, supraventricular tachycardia
- Gastrointestinal Disorders: gingival pain, upper gastrointestinal hemorrhage
- General Disorders and Administrative Site Conditions: chest pain, catheter site hemorrhage
- Hepatobiliary Disorders: cholecystitis
- Infections and Infestations: fungal infection, sepsis, bronchopulmonary aspergillosis, peridiverticular abscess, respiratory tract infection, pseudomonal lung infection, Mycobacterium avium complex infection
- Injury, Poisoning and Procedural Complications: post procedural pain, post procedural hemorrhage
- Nervous System Disorders: intracranial hemorrhage
- Psychiatric Disorders: mental status changes
- Renal and Urinary Disorders: renal failure, urethral hemorrhage
- Respiratory, Thoracic and Mediastinal Disorders: hemoptysis, lung infiltration, pulmonary embolism, respiratory arrest, pulmonary mass
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of DACOGEN. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
- Sweet's syndrome (acute febrile neutrophilic dermatosis)
- Differentiation syndrome
- Interstitial lung disease
7. Drug Interactions
Drug interaction studies with decitabine have not been conducted. In vitro studies in human liver microsomes suggest that decitabine is unlikely to inhibit or induce cytochrome P450 enzymes. In vitro metabolism studies have suggested that decitabine is not a substrate for human liver cytochrome P450 enzymes. As plasma protein binding of decitabine is negligible (<1%), interactions due to displacement of more highly protein bound drugs from plasma proteins are not expected.
8. Use In Specific Populations
8.4 Pediatric Use
The safety and effectiveness of DACOGEN in pediatric patients have not been established.
8.5 Geriatric Use
Of the total number of patients exposed to DACOGEN in the controlled clinical trial, 61 of 83 patients were age 65 years and over, while 21 of 83 patients were age 75 years and over. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out.
10. Overdosage
There is no known antidote for overdosage with DACOGEN. Higher doses are associated with increased myelosuppression including prolonged neutropenia and thrombocytopenia. Standard supportive measures should be taken in the event of an overdose.
11. Dacogen Description
Decitabine is a nucleoside metabolic inhibitor. Decitabine is a fine, white to almost white powder with the molecular formula of C8H12N4O4 and a molecular weight of 228.21. Its chemical name is 4-amino-1-(2-deoxy-β-D-erythro-pentofuranosyl)-1,3,5-triazin-2(1H)-one and it has the following structural formula:
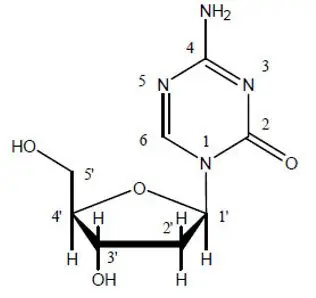
Decitabine is slightly soluble in ethanol/water (50/50), methanol/water (50/50) and methanol; sparingly soluble in water and soluble in dimethylsulfoxide (DMSO).
DACOGEN (decitabine) for injection, for intravenous use, is a sterile, white to almost white lyophilized powder supplied in a clear colorless glass single-dose vial. Each 20 mL vial contains 50 mg decitabine, 68 mg monobasic potassium phosphate (potassium dihydrogen phosphate) and 11.6 mg sodium hydroxide. Sodium hydroxide and/or hydrochloric acid are used for pH adjustment.
12. Dacogen - Clinical Pharmacology
12.1 Mechanism of Action
Decitabine is believed to exert its antineoplastic effects after phosphorylation and direct incorporation into DNA and inhibition of DNA methyltransferase, causing hypomethylation of DNA and cellular differentiation or apoptosis. Decitabine inhibits DNA methylation in vitro, which is achieved at concentrations that do not cause major suppression of DNA synthesis. Decitabine-induced hypomethylation in neoplastic cells may restore normal function to genes that are critical for the control of cellular differentiation and proliferation. In rapidly dividing cells, the cytotoxicity of decitabine may also be attributed to the formation of covalent adducts between DNA methyltransferase and decitabine incorporated into DNA. Non-proliferating cells are relatively insensitive to decitabine.
12.2 Pharmacodynamics
Decitabine has been shown to induce hypomethylation both in vitro and in vivo. However, there have been no studies of decitabine-induced hypomethylation and pharmacokinetic parameters.
12.3 Pharmacokinetics
Pharmacokinetic (PK) parameters were evaluated in patients. Eleven patients received 20 mg/m2 infused over 1 hour intravenously (treatment Option 2). Fourteen patients received 15 mg/m2 infused over 3 hours intravenously (treatment Option 1). PK parameters are shown in Table 3. Plasma concentration-time profiles after discontinuation of infusion showed a biexponential decline. The clearance (CL) of decitabine was higher following treatment Option 2. Upon repeat doses, there was no systemic accumulation of decitabine or any changes in PK parameters. Population PK analysis (N=35) showed that the cumulative AUC per cycle for treatment Option 2 was 2.3-fold lower than the cumulative AUC per cycle following treatment Option 1.
| Dose | Cmax
(ng/mL) | AUC0-INF
(ng∙h/mL) | T1/2
(h) | CL (L/h/m2) | AUCCumulative*
(ng∙h/mL) |
|---|---|---|---|---|---|
|
|||||
| 15 mg/m2 3-hr infusion every 8 hours for 3 days (Option 1)† | 73.8 (66) | 163 (62) | 0.62 (49) | 125 (53) | 1332 (1010-1730) |
| 20 mg/m2 1-hr infusion daily for 5 days (Option 2)‡ | 147 (49) | 115 (43) | 0.54 (43) | 210 (47) | 570 (470-700) |
The exact route of elimination and metabolic fate of decitabine is not known in humans. One of the pathways of elimination of decitabine appears to be deamination by cytidine deaminase found principally in the liver but also in granulocytes, intestinal epithelium and whole blood.
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis and Impairment of Fertility
Carcinogenicity studies with decitabine have not been conducted.
The mutagenic potential of decitabine was tested in several in vitro and in vivo systems. Decitabine increased mutation frequency in L5178Y mouse lymphoma cells, and mutations were produced in an Escherichia coli lac-I transgene in colonic DNA of decitabine-treated mice. Decitabine caused chromosomal rearrangements in larvae of fruit flies.
In male mice given IP injections of 0.15, 0.3 or 0.45 mg/m2 decitabine (approximately 0.3% to 1% the recommended clinical dose) 3 times a week for 7 weeks, decitabine did not affect survival, body weight gain or hematological measures (hemoglobin and white blood cell counts). Testes weights were reduced, abnormal histology was observed and significant decreases in sperm number were found at doses ≥0.3 mg/m2. In females mated to males dosed with ≥0.3 mg/m2 decitabine, pregnancy rate was reduced and preimplantation loss was significantly increased.
14. Clinical Studies
14.1 Controlled Trial in Myelodysplastic Syndrome
A randomized open-label, multicenter, controlled trial evaluated 170 adult patients with myelodysplastic syndromes (MDS) meeting French-American-British (FAB) classification criteria and International Prognostic Scoring System (IPSS) High-Risk, Intermediate-2 and Intermediate-1 prognostic scores. Eighty-nine patients were randomized to DACOGEN therapy plus supportive care (only 83 received DACOGEN), and 81 to Supportive Care (SC) alone. Patients with Acute Myeloid Leukemia (AML) were not intended to be included. Of the 170 patients included in the study, independent review (adjudicated diagnosis) found that 12 patients (9 in the DACOGEN arm and 3 in the SC arm) had the diagnosis of AML at baseline. Baseline demographics and other patient characteristics in the Intent-to-Treat (ITT) population were similar between the 2 groups, as shown in Table 4.
| Demographic or Other Patient Characteristic | DACOGEN N =89 | Supportive Care N =81 |
|---|---|---|
| Age (years) | ||
| Mean (±SD) | 69±10 | 67±10 |
| Median (IQR) | 70 (65-76) | 70 (62-74) |
| (Range: min-max) | (31-85) | (30-82) |
| Sex n (%) | ||
| Male | 59 (66) | 57 (70) |
| Female | 30 (34) | 24 (30) |
| Race n (%) | ||
| White | 83 (93) | 76 (94) |
| Black | 4 (4) | 2 (2) |
| Other | 2 (2) | 3 (4) |
| Weeks Since MDS Diagnosis | ||
| Mean (±SD) | 86±131 | 77±119 |
| Median (IQR) | 29 (10-87) | 35 (7-98) |
| (Range: min-max) | (2-667) | (2-865) |
| Previous MDS Therapy n (%) | ||
| Yes | 27 (30) | 19 (23) |
| No | 62 (70) | 62 (77) |
| RBC Transfusion Status n (%) | ||
| Independent | 23 (26) | 27 (33) |
| Dependent | 66 (74) | 54 (67) |
| Platelet Transfusion Status n (%) | ||
| Independent | 69 (78) | 62 (77) |
| Dependent | 20 (22) | 19 (23) |
| IPSS Classification n (%) | ||
| Intermediate-1 | 28 (31) | 24 (30) |
| Intermediate-2 | 38 (43) | 36 (44) |
| High Risk | 23 (26) | 21 (26) |
| FAB Classification n (%) | ||
| RA | 12 (13) | 12 (15) |
| RARS | 7 (8) | 4 (5) |
| RAEB | 47 (53) | 43 (53) |
| RAEB-t | 17 (19) | 14 (17) |
| CMML | 6 (7) | 8 (10) |
Patients randomized to the DACOGEN arm received DACOGEN intravenously infused at a dose of 15 mg/m2 over a 3-hour period, every 8 hours, for 3 consecutive days. This cycle was repeated every 6 weeks, depending on the patient's clinical response and toxicity. Supportive care consisted of blood and blood product transfusions, prophylactic antibiotics, and hematopoietic growth factors. The study endpoints were overall response rate (complete response + partial response) and time to AML or death. Responses were classified using the MDS International Working Group (IWG) criteria; patients were required to be RBC and platelet transfusion independent during the time of response. Response criteria are given in Table 5.
|
||
| Complete Response (CR) ≥8 weeks | Bone Marrow | On repeat aspirates:
|
| Peripheral Blood | In all samples during response:
|
|
| Partial Response (PR) ≥8 weeks | Bone Marrow | On repeat aspirates:
|
| Peripheral Blood | Same as for CR | |
The overall response rate (CR+PR) in the ITT population was 17% in DACOGEN-treated patients and 0% in the SC group (p<0.001) (see Table 6). The overall response rate was 21% (12/56) in DACOGEN-treated patients considered evaluable for response (i.e., those patients with pathologically confirmed MDS at baseline who received at least 2 cycles of treatment). The median duration of response (range) for patients who responded to DACOGEN was 288 days (116-388) and median time to response (range) was 93 days (55-272). All but one of the DACOGEN-treated patients who responded did so by the fourth cycle. Benefit was seen in an additional 13% of DACOGEN-treated patients who had hematologic improvement, defined as a response less than PR lasting at least 8 weeks, compared to 7% of SC patients. DACOGEN treatment did not significantly delay the median time to AML or death versus supportive care.
| Parameter | DACOGEN N=89 | Supportive Care N=81 |
|---|---|---|
|
||
| Overall Response Rate (CR+PR)* | 15 (17%)† | 0 (0%) |
| Complete Response (CR) | 8 (9%) | 0 (0%) |
| Partial Response (PR) | 7 (8%) | 0 (0%) |
| Duration of Response | ||
| Median time to (CR+PR) response - Days (range) | 93 (55-272) | NA |
| Median Duration of (CR+PR) response - Days (range) | 288 (116-388) | NA |
All patients with a CR or PR were RBC and platelet transfusion independent in the absence of growth factors.
Responses occurred in patients with an adjudicated baseline diagnosis of AML.
14.2 Single-arm Studies in Myelodysplastic Syndrome
Three open-label, single-arm, multicenter studies were conducted to evaluate the safety and efficacy of DACOGEN in MDS patients with any of the FAB subtypes. In one study conducted in North America, 99 patients with IPSS Intermediate-1, Intermediate-2, or high-risk prognostic scores received DACOGEN 20 mg/m2 as an intravenous infusion over 1-hour daily, on days 1-5 of week 1 every 4 weeks (1 cycle). The results were consistent with the results of the controlled trial and are summarized in Table 8.
| Demographic or Other Patient Characteristic | DACOGEN N =99 |
|---|---|
| Age (years) | |
| Mean (±SD) | 71±9 |
| Median (Range: min-max) | 72 (34-87) |
| Sex n (%) | |
| Male | 71 (72) |
| Female | 28 (28) |
| Race n (%) | |
| White | 86 (87) |
| Black | 6 (6) |
| Asian | 4 (4) |
| Other | 3 (3) |
| Days From MDS Diagnosis to First Dose | |
| Mean (±SD) | 444±626 |
| Median (Range: min-max) | 154 (7-3079) |
| Previous MDS Therapy n (%) | |
| Yes | 27 (27) |
| No | 72 (73) |
| RBC Transfusion Status n (%) | |
| Independent | 33 (33) |
| Dependent | 66 (67) |
| Platelet Transfusion Status n (%) | |
| Independent | 84 (85) |
| Dependent | 15 (15) |
| IPSS Classification n (%) | |
| Low Risk | 1 (1) |
| Intermediate–1 | 52 (53) |
| Intermediate–2 | 23 (23) |
| High Risk | 23 (23) |
| FAB Classification n (%) | |
| RA | 20 (20) |
| RARS | 17 (17) |
| RAEB | 45 (45) |
| RAEB-t | 6 (6) |
| CMML | 11 (11) |
| Parameter | DACOGEN N=99 |
|---|---|
|
|
| Overall Response Rate (CR+PR) | 16 (16%) |
| Complete Response (CR) | 15 (15%) |
| Partial Response (PR) | 1 (1%) |
| Duration of Response | |
| Median time to (CR+PR) response - Days (range) | 162 (50-267) |
| Median Duration of (CR+PR) response - Days (range) | 443 (72-722†) |
16. How is Dacogen supplied
DACOGEN for injection is a sterile, white to almost white lyophilized powder for intravenous use supplied as:
- NDC 59148-046-70, 50 mg single-dose vial individually packaged in a carton.
| DACOGEN
decitabine injection, powder, lyophilized, for solution |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - Otsuka America Pharmaceutical, Inc. (008314390) |






