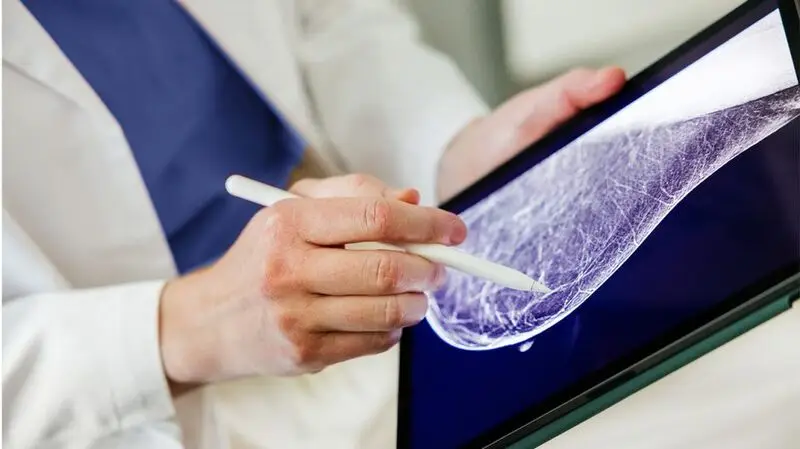
- A study suggests that an artificial intelligence (AI) tool can analyze routine mammogram images to measure a marker associated with cardiovascular disease.
- Individuals with this marker had a significantly higher risk of future cardiovascular events, with some having roughly two to three times higher risk of major cardiovascular disease.
- As many people already undergo mammography for breast cancer screening, AI analysis of these images could potentially help identify cardiovascular risk without additional tests, enabling earlier prevention strategies.
Heart disease is the
Despite
Mammograms are crucial for detecting breast cancer and often serve as a first-line method for routine breast cancer screening.
Guidelines for screening usually vary depending on an individual’s risk. However, recommendations
Most people may think that mammograms only identify breast cancer. However, new research published in the European Heart Journal, suggests an AI tool may be able to detect the risk of developing serious heart disease by analyzing routine mammograms.
Researchers say the approach could turn a widely used breast cancer screening tool into a way to also identify those at risk of cardiovascular disease.
In the new study, researchers developed an AI tool capable of measuring the amount of calcium in breast arteries from standard mammogram images.
This condition is known as
The researchers analyzed data from 123,762 women who underwent breast cancer screening and had no known cardiovascular disease at the start of the study.
Using the AI tool, the team categorized the amount of arterial calcification visible in the mammograms as absent, mild, moderate, or severe. They then compared these findings with later records of cardiovascular events such as heart attack, stroke, heart failure, or death from heart disease.
The results showed a clear relationship between the amount of calcification and the likelihood of developing serious cardiovascular disease.
Notably, females with mild calcification were about 30% more likely to experience serious cardiovascular disease compared with those with none. Those with moderate calcification had a more than 70% higher risk, while those with severe calcification had two to three times the risk.
The association remained even after accounting for other known risk factors, such as diabetes and smoking.
Lori Daniels, MD, FACC, a board-certified cardiologist and professor of medicine at UC San Diego School of Medicine was not surprised by the strength of the association between BAC and future cardiovascular events.
Her group previously published similar findings, highlighting an association between higher BAC levels and heart disease risk.
“The present study is in that ballpark – their age-adjusted model is almost identical in magnitude,” Daniels said.
“Our 2024 UC San Diego study also showed that BAC was particularly informative in younger women. This is important because younger women are the ones least likely to already know that they are at increased cardiovascular risk.”
Importantly, the findings of the study observe that the relationship between breast arterial calcification and cardiovascular risk is also present in females under the age of 50, a group often considered to be at lower risk of heart disease.
The results indicate that the more calcium visible in breast arteries on a mammogram, the greater the risk of a future cardiovascular event.
As many females already undergo routine mammography, the technique could reveal cardiovascular risk earlier than traditional screening methods and provide heart health insights without requiring additional tests or procedures.
Implementing the approach would involve integrating the AI tool into imaging systems and developing guidelines for notifying clinicians and patients about cardiovascular risk findings.
If integrated into clinical practice, AI-based analysis of mammograms could prompt earlier discussions between individuals and doctors about preventive strategies, such as cholesterol testing, lifestyle changes, or medication.
“Excellent question, and the subject of an upcoming publication of mine – we are evaluating women with and without traditional cardiovascular risk factors.
The short answer is that I suspect BAC will be useful in both groups to further refine risk, though absolute risk is always higher in groups with higher baseline risk.
One might argue that if a woman is already at increased risk, how can this be helpful? Although I think the biggest public impact will be in identifying risk in those women who do not already know they are at risk (bringing it to their attention, for instance, and perhaps then identifying other risk factors).
I still see value in women who do know they are at risk. Simply seeing a visual image of the calcium buildup in the breast arteries could potentially sway younger women to take their cardiovascular health more seriously, and make positive changes.”
– Lori Daniels
In an accompanying editorial by Daniels, experts note that many females regularly receive mammograms but do not know their cholesterol levels, which are a major cardiovascular risk factor.
Using mammography to also assess heart disease risk could help close this gap and identify those who might otherwise go undiagnosed.
However, the authors note that further research and clinical trials are necessary before the technology can be widely implemented.
Additionally, the authors highlight that as an observational study, the research can only demonstrate an association between breast arterial calcification and cardiovascular disease risk, rather than proving a direct cause-and-effect relationship.
Future studies will aim to test whether using AI-based mammogram analysis in routine care actually improves prevention and outcomes for cardiovascular disease.
I am hopeful that mammograms will ultimately become a dual screening tool for both breast cancer and CVD risk, and that we will some day look back and say why in the world were we not utilizing this ‘free’ information sooner?
It currently takes some degree of either time or money (or both) to get a reliable BAC reading from a mammogram – either the radiologist needs to carefully review the study and identify calcium in the artery (and not in the fat or other breast tissue) – or an automated model needs to do so.
Currently, this is available in a commercial, FDA-cleared product that is inexpensive but not free. Still, the information is sitting there, and it is clearly related to cardiovascular outcomes; I imagine that as more women become aware of this, we will reach a point in time where women are demanding access to this information.
As for the workflow, once radiologists begin to routinely report BAC (at least in women under a certain age – perhaps 65 or so), I think the next step is simply getting primary care physicians (PCPs) educated about this, and having them comprehensively address cardiovascular risk in women with BAC.
Most of this can be handled by PCPs. When they identify additional risk factors, then cardiology referral and/or additional imaging could be warranted. None of this would require large workflow changes.
– Lori Daniels, MD, FACC
“I think the first steps should be a comprehensive cardiovascular risk assessment by the PCP — identifying risk factors for both atherosclerotic disease as well as heart failure.
If additional risk factors are found, they should be addressed with lifestyle and/or medication as indicated; and if there is concern for particularly high risk, then additional cardiovascular testing and/or imaging could be considered.”
– Lori Daniels, FACC





